This article is written in partnership with Yarlap®—they’re dedicated to helping us enjoy the benefits of better pelvic floor health and we’re honored to work with them. ~ ed.
~
Some call it the bottom of a cereal bowl. Some call it a hammock. Or an Anchor.
Whatever metaphor you want to use to describe it, there’s a group of muscles around both men’s and women’s pelvic regions. This band of muscles is called your pelvic floor, and it can either do us a whole lot of good (keep unwanted accidents at bay and help us have better orgasms), or cause us a whole bunch of trouble—our bladders can start to slip through our vaginas, literally; it’s called pelvic prolapse.
Your pelvic floor should be your friend—your very. good. friend.
The problem? Many of us don’t know where to find this posse of pelvic pals, nonetheless how to meet them, treat them, and properly greet them with that just-right “handshake” that’s sure to forge a right but not-too-tight bond of collaboration (aka a proper Kegel).
So let’s get to it, shall we?
Try this and prepare to be (pelvic) floored by the results >>
What exactly is the pelvic floor?
The pelvic floor spans between your pelvic bone in the front of your body and your tailbone, and also extends between your sit bones.
It’s located at the base of the abdomino-pelvic cavity, which is just a fancy way of saying that it’s called the pelvic floor and not, say, a roof, for the reason that, you know, it’s all the way at the bottom of the cavity that houses our pelvic organs.
According to one study, there is apparently a little drama and “significant controversy with regards to the nomenclature,” (1) so, depending on where you look, or what you’re trying to understand about the pelvic floor, there are either three or fifteen muscles (2) that make up this powerhouse of a crew.
For the purposes of illustrating just how important our pelvic floors are, we’ll go with 15, and we’ll add that there are also 20 ligaments in the pelvic floor—22 for people with penises. But for brevity’s sake, the three major players are pubococcygeus, puborectalis and iliococcygeus.
So, now you know their names, but it sounds like you’re in a foreign country. Let’s take you there to meet them.
Where is the pelvic floor?
Let’s get physical.
If you are a visual person, and you’re, um, close with yourself—you can take a mirror down there and have a look at some of the great work they do as a team.
1. Observe the look of your pelvic region (pubic region to your anus) when simply relaxed.
2. Now, slowly tighten your muscles as if you were trying to hold in some urine or gas. You should see a tightening or drawing in of the whole region as your pelvic floor muscles contract.
3. Relax again.
4. Then push out a little bit (just a bit lighter than during an easy bowel movement). You should see the region open up slightly.
This is probably the best ‘not’ sex toy ever >>
If you’re more tactile and would prefer to perhaps keep all your clothes on, you can:
1. Sit on the floor.
2. Reach down and lightly place your finger tips somewhere in the space between your two sit bones (you don’t have to go too far center, don’t worry).
3. Tense up as if you were holding in some urine and feel the muscles move just slightly up from your fingertips.
4. Relax and feel them in their natural state.
5. Cough or sing to feel them protrude to press a little more firmly against your fingertips.
There. Now you’re properly acquainted.
What does the pelvic floor do and why is that important?
Let’s cut right to the chase: Pelvic floor strengthen helps with:
>> Making sex better
>> Stopping bladder leaks
>> Postpartum care
Just like the floor beneath your feet right now supports everything resting atop it, your pelvic floor does the same and supports your pelvic organs, including the vagina, uterus, prostate, rectum, bladder, and urethra.
If your pelvic floor muscles were to weaken, everything above might start to slip into the space where the floor began to sag. And when things relocate in our bodies, that can cause dysfunction and pain.
It’s the same on the flip side; though it’s less common, the pelvic floor can also be overactive and too tight, which can lead to similar issues.
How do I know if I’m in my pelvic floor’s friend zone?
This moment sticks out in my mind: A friend’s family and I were headed to see Titanic when, as we walked through the parking lot, her mom sneezed and made some quiet comment about how she’d “piddled” again. I, a middle schooler at the time, exclaimed pridefully that I had a bladder of steel, to which the mother replied with these words:
“Just wait ‘til you have children.”
So, I thought that’s what happens when women have babies—and only after they have babies.
Welp, I’m 36 and childless, and despite that I don’t have little ones, when I sneeze, I piddle. When I cough hard enough, I piddle. Sometimes during sex, I’m not sure if I’m squirting or…you get the point.
Speaking of “squirting,” the quality of our orgasm is directly affected by the quality of our pelvic floor tone. That’s because the clitoris runs directly along the pelvic floor muscles (3), which is why you’re likely to see Kegels mentioned everywhere for sexual pleasure. The muscles of the pelvic floor are the same ones that contract during orgasm, which means if they’re weak, so will be your (not so) big O.
They’ve done their homework and are medically and Elephant-approved! >>
The bottom line (no pun intended) is that it’s a myth that only mothers struggle with pelvic floor dysfunction, which is essentially any less-than-optimal function of the pelvic floor muscles—including no control at all.
In actuality, at some point in life, whether we like it or not, we’re all—women of all ages, athletes, and even men—going to lose some degree of control of our pelvic floor. It’s just the science of aging.
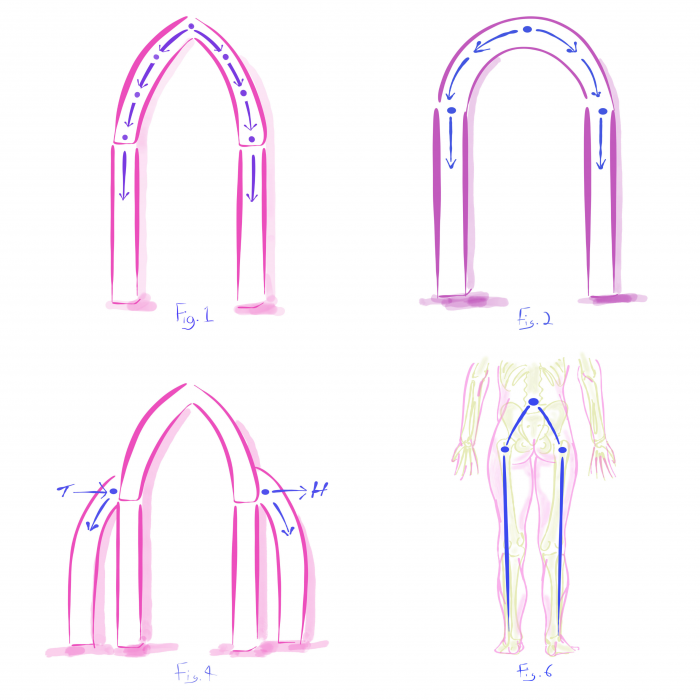
Imagine an old cathedral with its Gothic arch. That’s your pelvic region. Depending on the cathedral, flying buttresses or chains support the arch and mitigate the stress placed on it. Those are your pelvic floor muscles.
As time goes by and we age, those metaphorical buttresses begin to deteriorate, or our chains loosen without reinforcement. Our Gothic arch begins to sag and cause structural problems that can affect our bodies at large in a variety of ways:
>> Urinary incontinence
>> Stress incontinence (loss of urine when coughing, sneezing, or exercising)
>> Pelvic pain
>> Feelings of incomplete emptying of bladder and/or bowel
>> Difficulty with bowel control
>> Stubborn belly pudge
>> Pelvic organ prolapse (where pelvic organs fall out of our pelvis)
>> Pain during sex and/or orgasm
>> Painful urination
>> Lower back pain or hip pain, with no other cause (more common in the athletic population)
>> Testicular pain
>> Inguinal and pelvic pain
That’s quite the load.
So, how can I get my pelvic floor to—err, have my back?
For us women, it can sometimes feel as if we’re set up for disaster when it comes to the more common issue of poor pelvic tone.
So many things are thrown at us that cause these issues: trauma, pregnancy, childbirth, hormones, menopause, being active, not being active enough, weighing too much or weighing too little…the list goes on. Heck! Even COVID is on that list due to quarantine’s tendency to promote sedentary habits, and increase stress and anxiety—all of which contribute to pelvic floor dysfunction (4).
“The pelvic floor muscle is weird because it can be loose or it can be way too tight. It’s kind of like Goldilocks and the Three Bears. You have to find out where it’s just right,”(5) says MaryEllen Reider, a leading voice in the pelvic floor and sex tech wellness space and co-director of Yarlap®, a wellness device that treats urinary incontinence and improves sexual performance and experience through the company’s AutoKegel® technology.
In other words? We basically have to fall into a very small area to have the perfect pelvic floor; otherwise we have to work to maintain that perfect tone.
So, we may want to jump into doing those Kegels that we’ve all heard help with this sort of an issue. But there’s a problem with that: Proper pelvic floor function and health isn’t about just toning (as is the primary focus of Kegels), it’s about striking the right balance between all muscles involved.
And even if it were just about Kegels, Reider reminds us that Kegel exercises are extremely difficult to do on their own. Up to 70 percent of women are unable to do a Kegel properly unless shown how by a medical professional (6), and beyond that, some women may have atrophy so advanced that they do not have control of their pelvic floor muscles at all.
Fortunately, muscles can be re-educated and that’s where Yarlap comes in.
Yarlap is an award winning, FDA approved e-stimulation device that precisely targets and tones the pelvic floor muscles through a series of six preset 20-minute toning programs. And the best part about it is that whether you have the need to maintain pelvic control or have atrophy with zero control, Yarlap has your back.
When we know that we’re under-toned, we can literally sit back, relax, and let Yarlap’s AutoKegel Technology do the work for for us —and with flawless form.
50 percent of women can’t do a Kegel correctly. But you can. >>
But it’s only recommended for use if we’re certain that we’re on the under-toned end of the pelvic floor spectrum. And sometimes that can be hard to tell.
Experts like Reider are quick to point out that if you’re seeing signs of pelvic floor issues and you’re able, you should aim to get in for a medical consultation—particularly if you feel you might be on the too-tight end of things.
“If you feel pain, and [the muscle is] tightened, and you can go to a doctor, instead of doing Kegel exercises which clench your muscles, it’s recommended that you do pelvic floor relaxation—a massage program—to release the tension down there,” says Reider. “You don’t want to be doing Kegel exercises because that’s just going to clench an already clenched muscle.”
And there are other preventative actions we can take to help prevent the progression of poor pelvic floor health, according to Mary Austin, director of the Pelvic Health Physical Therapy Residency at Johns Hopkins Hospital and Alicia Jeffrey-Thomas, a pelvic floor physical therapist at Greater Boston Urology as shared in The Washington Post:
> When you use the bathroom, focus on relaxing rather than pushing, which can create pressure.
>> Perhaps invest in a squatty potty—or make sure your knees are positioned a little higher than your hips to create more length in the pelvic floor muscles and help yourself poop easier.
>> Sip water instead of chugging it.
>> Minimize drinking caffeinated or carbonated beverages.
>> Avoid sitting in one position for hours on end to avoid cumulative, low strain.
 Here’s the clincher: Pelvic floor health doesn’t have to be this mysterious, secretive, or scary thing that we avoid talking about.
Here’s the clincher: Pelvic floor health doesn’t have to be this mysterious, secretive, or scary thing that we avoid talking about.
While incontinence and poor pelvic tone may not be quite normal from a medical perspective, it is common, and should be a part of common discussion—especially with our health providers and the young women in our lives as they grow into adulthood.
When we discuss what is going on in our bodies and come to have a greater understanding of their inner structure and workings, we are able to take a more balanced approach to minor symptoms as they arise and partake in preventative care.
We take the power into our own hands (or pelvic floor muscles) and fully grasp onto our wellness.
~
References:
(1) NCBI.nlm.nih.gov
(2) Physiopedia.com
(3) Scitechnol.com
(4) The Washington Post
(5) Honeydew Me Podcast
(6) pubmed.ncbi.nlm.nih.gov



Read 8 comments and reply