Elephant is not your doctor or hospital. Our lawyers would say “this website is not designed to, and should not be construed to provide medical advice, professional diagnosis, opinion, or treatment to you or any other individual, and is not intended as a substitute for medical or professional care and treatment. Always consult a health professional before trying out new home therapies or changing your diet.” But we can’t afford lawyers, and you knew all that. ~ Ed.
~
I discovered that belly breathing exacerbated my condition. This is the simple change I made—and so can you.
I’ve struggled—and maybe you have, too—with acid reflux for years. GERD, to be specific: GastroEsophageal Reflux Disease, or perpetual heartburn. My gastroenterologist informed me that as we age, the esophageal sphincter can become “floppy” (hmm, what a pleasant image) and fail to seal the gateway between the esophagus and the stomach properly. This results in acid rising up into the gullet and causing an intense burning sensation. In addition to the searing pain, it can lead to serious problems if not treated, including cancer (yikes!).
Looking for a cure.
If you’ve been through this challenging condition, your doctor, like mine, probably suggested Prilosec or a similar medication. I resisted that for a while, as I hate taking meds. The first month I was burning so badly in my esophagus that I slept (or attempted to) in the recliner in the living room, so that the acid didn’t gurgle up into my throat when I laid down. At times, I could feel the burning into my ears.
I went to many, many natural medicine practitioners: chiropractors, Ayurvedic practitioners, acupuncturists, naturopaths, osteopaths, homeopaths. You’ve probably been through the same routine. Each one helped a little, but none of them cured me.
A surprising connection.
However, one of them—I wish I could remember who—said something that surprised me. She said that one of the causes of acid reflux is breathing.
Of course, she didn’t mean breathing in general, or else I would be in trouble, eh? She meant that a certain way of breathing creates suction that pulls the acid up the esophagus.
I dismissed it in the moment—after all, I’ve been a yoga teacher for over 25 years, and I thought I knew something about breathing. But after I left her office, I considered it. Could there be something about the yogic breathwork I usually practice that was exacerbating my condition?
A search of the internet about this topic turned up zilch. There were plenty of articles about how deep breathing can help relax you and ease GERD, but nothing about how the way that we breathe might be problematic and actually aggravate acid reflux.
Bedtime Observations.
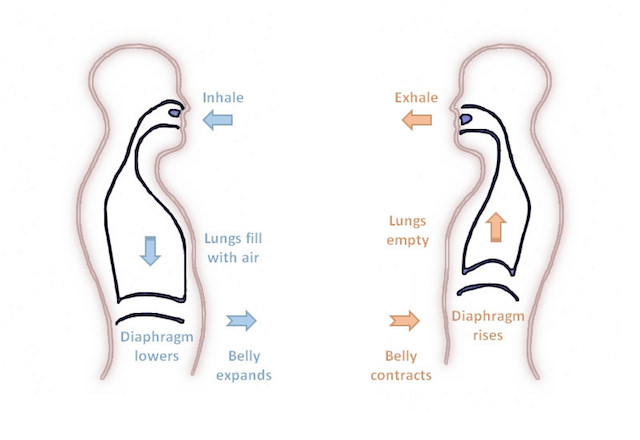
So I started observing myself. Going to bed at night was the worst time for my reflux, due to my reclined position. As usual, I engaged in belly breathing. The way I was taught this in my early years of practicing yoga was referred to as “three-part breath,” also known as Dirgha Pranayama. You probably regularly practice this in your own yoga classes. You begin with breathing down into the belly, filling the abdomen, then letting the breath continue to rise up through the rib cage to lastly fill your upper lungs near the collarbones. Then, you exhale slowly and deliberately in reverse, emptying the belly last.
Gurgle gurgle. My stomach acid was getting a bit stirred up. And as I continued to practice and observe, I found that when I felt a small gurgling sensation and did this three-part breath, the gurgling would intensify. And I couldn’t get the gurgling to stop when I breathed into my belly first.
This posed a bit of a problem. I really liked belly breathing to help me go to sleep. It engages the parasympathetic nervous system and helps the body and mind to relax. But I could clearly see that there was some connection between this way of breathing and the activity of the stomach acid in my esophagus. I wondered if there was a way to continue breathing into my abdomen, but not stir things up.
Finding a Different Way to Breathe.
Logically, if going from the bottom up was pulling this fluid up and out of my stomach, perhaps I could reverse the process. I’d still be able to extend my diaphragm downward to release in the belly, but I’d start at the top instead. I inhaled into my upper chest first, then down into my stomach, and lastly into my lower abdomen.
After a few rounds, I began to get the hang of it. And I noticed less reflux happening! The more I worked with it, the more I could control the reflux activity. If I heard gurgling happening, I’d pause and wait until it settled a bit; then, I’d practice this “reverse three-part breath.”
Bedtime became easier, and I attained some control over my reflux symptoms.
I also found that Ujjayi Pranayama––the style of yogic breath that makes a sound like the ocean by constricting the throat slightly—creates a similar suction action. So I focused instead on controlling my length of inhale and exhale through more subtle means, with a quiet, soft breath. Again, the reflux improved.
Reflux-Free (Mostly)!
These changes in my intentional Pranayama—and even in just my ordinary way of breathing—have been part of a full health regimen (that involves adhering to a mindful diet, taking specific supplements, and engaging in stress management practices) that has brought me to where I am today: mostly reflux-free.
Of course, this is totally anecdotal, but it has worked for me and it might for you. It takes a little more skill to practice three-part breath in reverse, as most of us tend to breathe solely into the chest and find it challenging to extend the diaphragm into the abdomen.
However, if you have endured this painful disease like I have, give it a try. At the very least, you’ll learn something about your condition and a lot about how you breathe. Share your experiences here and what has worked for you!
Author: Rev. Connie L. Habash
Image: Remedial Class/Flickr
Editor: Callie Rushton
Copy Editor: Catherine Monkman






Read 0 comments and reply