
*Editor’s Note: Elephant is not your doctor or hospital. Our lawyers would say “this web site is not designed to, and should not be construed to provide medical advice, professional diagnosis, opinion, or treatment to you or any other individual, and is not intended as a substitute for medical or professional care and treatment. Always consult a health professional before trying out new home therapies or changing your diet.” But we can’t afford lawyers, and you knew all that. ~ Ed.
~
I’ve been quarantined.
I received a call last night notifying me that a patient I had come into direct contact with had “preliminary” tested positive for the Coronavirus. I was instructed to stay out of work for 14 days in “self-quarantine” and to monitor for any symptoms.
I’m not symptomatic yet, and despite the media, I’m not scared.
What I am, however, is concerned that the general public lacks the knowledge that it so desperately needs.
Here are the top seven Need to Knows:
1. What a virus is:
A virus is a parasitic organism 1,000 times smaller than bacteria. They invade the cells in the body in hopes of taking over completely, moving from one host cell to the next.
2. How our bodies fight viruses:
The “sickness” that we feel are symptoms of the disease. This is the body’s way of fighting off the invaders and how it works to build natural immunity. It keeps us from getting sick with the same virus again.
Incubation periods vary from virus to virus, but generally we would start to notice symptoms within 24-48 hrs.
Fevers are a good thing. Let the body work its magic—just monitor how high the temperature gets. Personally, I wouldn’t take a fever reducer until the fever reaches 101. Do not wrap in blankets and/or add clothing. Turn the heat down inside the house if possible.
Stay hydrated. This is of the utmost importance.
3. Viruses mutate:
Viruses are intelligent organisms. They are continuously evolving and fighting for survival. Because some reproduce so quickly, this gives them the upper hand in the evolutionary chain. The perfect example of this is influenza. There are over 29 different Flu A viruses, and this isn’t including Flu B. This is why it is so important to know which viruses are in the flu vaccines that we receive—we can still get the flu, even after getting the shot.
Many of the mutations have no noticeable effect. But every once in a while, one might help the organism to survive—for example, by letting viruses infect not just birds, but people, too.
*Side note: even among viruses there’s a wide variation in mutation rates. Some viruses are more stable than others. This is why we’re protected against the measles virus even though were vaccinated years ago.
4. Coronavirus COVID-19:
Coronaviruses are a large family of viruses that cause illness ranging from the common cold to more severe respiratory illnesses. They are zoonotic, meaning they are transmitted between animals and people. COVID-19 is in the same family as Middle East Respiratory Syndrome (MERS-CoV), which was transmitted from camels, and Severe Acute Respiratory Syndrome (SARS-CoV), which was transmitted from civet cats. The reason everyone is freaking out is because this is a new strain and we have yet to discover where it comes from, there are no preventative measures in place such as a vaccine, nor are most medical facilities prepared for testing.
With this specific virus, signs and symptoms may appear 2-14 days after exposure.
Watch out for:
Fever
Cough
Shortness of breath
5. Testing:
According to the CDC, there are a few ways to test for COVID-19.
>> Swab. A health care provider will use a special swab to take a sample from your nose and throat.
>> Nasal aspirate. A health care provider will inject a saline solution into your nose, then remove the sample with gentle suction.
>> Tracheal aspirate. A health care provider will put a thin, lighted tube called a bronchoscope down your mouth and into your lungs, where a sample will be collected.
>> Sputum test. Sputum is a thick mucus that is coughed up from the lungs. You may be asked to cough up sputum into a special cup, or a special swab may be used to take a sample from your nose.
>> Blood. As far as I know, the only testing measures being used thus far (in my area and surrounding areas) are either sputum testing or nasal aspirate. The samples are then sent out to a different facility to be processed. Time and duration of results received depend on the facility and type of testing.
6. Treatment:
There are not any known cures for a virus. Health care providers can only treat your symptoms, and usually do this with antivirals. Given the newness of COVID-19, there aren’t any antivirals for health care providers to prescribe.
Don’t panic.
What most people don’t realize is that antivirals are only effective within the first 48 hours of exposure—not 48 hours from when we become symptomatic. By the time we become symptomatic, it’s too late for the antivirals to work. The best thing we can do in this situation is to take ibuprofen and stay hydrated while we’re lying in misery.
I know the general public is concerned about the mortality rates of COVID-19. What the media is not telling us is the demographics of these deaths. For instance, just as with the flu virus, mortality rates are increased due to secondary infections, and not the virus itself. Once the immune system has been compromised, or other disorders have weakened the body, it’s much easier for other invaders to enter our bodies, too.
Secondary infections are what we should be looking out for. On average, the disease lasts two weeks. If you notice any change in your signs or symptoms during this period, then go see your health care provider. You should be getting better, not worse.
7. Prevention:
>> Soap is more effective than hand sanitizer. The method and length of time matter. They teach health care workers to sing “Happy Birthday” twice while scrubbing up to the wrists and underneath fingernails. Use warm to hot water.
>> Hand sanitizer is better than nothing.
>> The face masks they are providing are not going to prevent a virus from entering your body. Most of the time, the masks worn by health care professionals are the same ones provided for the public. The only exception is the N-95 mask, which must be specifically fitted to a person’s face and then tested for accuracy. Other than this one exception, a mask is not going to stop a virus.
>> Stop touching your face. Even if you don’t come in direct contact with someone who has the virus or someone who is a carrier, you can pick up the virus from an object. This is the quickest way diseases are spread—through your mucus membranes. It’s called the “first line of defense” for a reason.
>> Cover your coughs, but don’t use your hands. When you go to cough, raise your arm and cough into your shoulder. This prevents spreading through the hands onto other objects.
>> Teach other people. We need to help each other, not live in fear of one another.
Unfortunately, there is nothing that can be done—in this period of time—to stop the spread of COVID-19. I’m not telling you this to scare you, but rather prepare you.
There are going to be some of us who are just carriers—those of us who show no signs or symptoms, but the virus uses us as an Uber, hopping from one person to the next. Others among us will get sick, and some of us will die. Knowledge is our only power. Use it wisely.
~
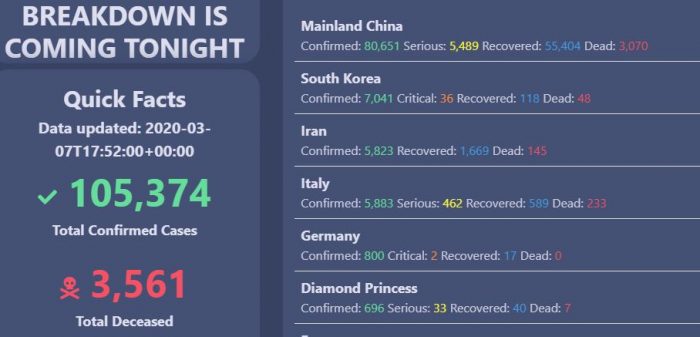
17-year-old Avi Schiffmann created a website that tracks the spread of the coronavirus.
See Avi’s updated coronavirus dashboard.
~
Editor’s note: I’ve always been partial to the Namaste greeting myself.
~

 Share on bsky
Share on bsky




Read 11 comments and reply